Diyya never thought the treatment plan for her chronic and debilitating stomach pain would be a small device behind her ear.
She’d been traveling with her family when everyone came down with food poisoning. Hers just never seemed to run its course.
“Something still just felt a little bit off,” she says.
A few months later, she fainted during a cooking class — but since she has a family history of fainting, she wasn’t too concerned. Despite taking it easy and resting, Diyya’s stomach pain persisted, and she experienced rapid weight loss.
She started seeing a variety of gastroenterologists ― doctors who specialize in the digestive system ― and received a slew of potential diagnoses, ranging from lactose intolerance to stomach paralysis, a condition that prevents the stomach from emptying its contents properly and often causes nausea and vomiting.
Diyya’s stomach pain started affecting her day-to-day life. She was throwing up several times per week, and some days she was too sick or weak to leave the house. Diyya missed so much school that she needed special accommodations for schoolwork and standardized testing.
She also stopped eating flavorful foods she’d once enjoyed and stuck to plain foods like rice and roasted vegetables.
“I got used to eating bland food,” Diyya says. “I would rather eat boring food than eat something good and be sick.”
The quest for a diagnosis
Eventually, Diyya and her parents were referred to Dr. Jeffrey Ho, a pediatric gastroenterologist at CHOC. He recognized that Diyya’s problem was related to the muscles in her digestive track and ordered an upper endoscopy, also called an esophagogastroduodenoscopy or EGD, to get a better idea of what was causing Diyya’s pain.

To perform an EGD, the doctor uses a long, flexible lighted tube called an endoscope. The endoscope is guided through the patient’s mouth and throat, then through the esophagus, stomach and the first part of the small intestine called the duodenum. The physician can examine the inside of these organs and detect abnormalities. Through the endoscope, the physician can also insert instruments to get samples for a biopsy. Diyya’s EGD and biopsy were normal.
She tried a few different herbal and traditional medicines, but nothing seemed to alleviate Diyya’s pain and symptoms. Hypnotherapy was helpful, but her main issues of stomach pain and nausea persisted.
A diagnosis and a path forward
Diyya was ultimately diagnosed with functional abdominal pain, meaning there’s a disconnect between the way her brain and gut communicate. She was also diagnosed with an allergy to barley and found that eating gluten contributed to her vomiting. Since her functional abdominal pain was accompanied by constipation or diarrhea, it is considered irritable bowel syndrome or IBS.
Diyya started working with Dr. Ashish Chogle, a pediatric gastroenterologist at CHOC.

“A lot of patients with functional abdominal pain have been told by physicians elsewhere that their pain is all in their head. That they’re just anxious. I tell them it’s true pain,” Dr. Chogle says. “For the first time, a doctor is justifying their pain and giving them a path forward.”
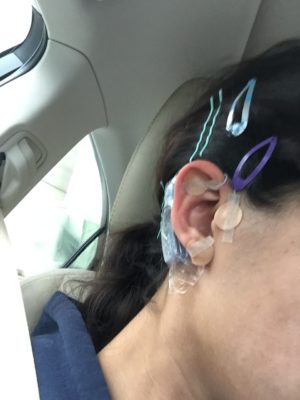
Diyya’s path forward was something called neuro-stimulation, or neuro-stim—through the IB-stim, a small device placed behind her ear. Subtle electrical pulses originate in this device and travel through short wires and into needles attached to nerves in the ear. These gentle stimulations target nerves and aim to relieve chronic and acute pain. The IB-Stim is a non-drug alternative for acute and chronic pain that alters the way pain pathways function.
“It’s rewriting the nerves and helping my stomach pain feel better,” she says.
Neuro-stimulators are applied in a clinical setting, and remain active for a few days, while the patient resumes normal activity. On the fifth day, the patient removes the neuro-stim at home. On day seven, they return to the clinic and a new device is applied. This process typically repeats four times, for a month-long course.
Diyya felt tiny pulses behind her ear the day after her neuro-stim was applied.
“The cool thing about neuro-stim is that your ears get used to the pulses,” Diyya says. “You notice it at first, but then you don’t notice it after an hour or so.”
The benefits of neuro-stimulation
A week later, Diyya was already feeling better than she had in a year.
“What I would’ve taken for granted before, suddenly became achievable again,” she says. “First, I could bend over and tie my shoe without pain. Then I could go for a walk, and even go back to a full day of school.”
Diyya began to put on weight — a good thing, since she had lost weight from eating a minimal, bland diet. She was strong enough to start physical therapy, a necessary part of rebuilding her strength, since her muscles had atrophied from a lack of physical activity.
“Finally, I could eat more normal food again. I could start becoming more active. I felt like I was finally getting back to normal,” Diyya says.
Diyya began neuro-stim around the same time as another teenage patient, and they were able to swap tips and bond amidst a shared experience. Their moms did, too.
“Since your neuro-stim can’t get wet, it’s tricky to wash your hair,” Diyya says. “I’d been using a shower cap, and she had found a great dry shampoo. I brought her my favorite shower cap, and she brought me her favorite dry shampoo.”
Diyya’s mom, Priya, had a hard time seeing her daughter struggle and was comforted by meeting another mom who understood what she was going through.
“As a mom, it was very hard to see Diyya deteriorate right before our eyes. We went from having an active child who loved to eat to a child who was so weak that she couldn’t get up to go to school,” Priya says. “It felt like, as parents, we were on the journey alone. When I met another patient’s mom at the neuro-stim placement appointment, it was so wonderful to have someone to talk to who understood what we were going through. We exchanged information about different providers and tips for managing school absences.”
The device, approximately 1 ½ -inches in size, is discreet.
“I always wear my hair up, and anyone who did notice my neuro-stim assumed it was a hearing aid,” Diyya says. “When anyone at school asked about it, I was able to educate them about this really cool technology that they’d never heard of before.”
Getting back to her old self
In addition to seeing physical benefits from her neuro-stim treatment, Diyya is getting back to her old self.
“Diyya is a new person after this experience. This experience has definitely taught her what the word resilience means. Before she was sick, everything from grades to sports came easily for her,” Priya said. “She is still working on accepting of her new normal. Sometimes she misses being able to eat whatever she wants or exercise without fatiguing.”
A talented musician, Diyya was able to join her school’s marching band, an activity she “wouldn’t even have thought possible” when she was sick, she says.
Sticking to a schedule also helps her feel her best. Starting high school and a new schedule led to a flare up of pain, so she did a second course of neuro-stim and is now back on track.
“For me, the level I’m at right now is wonderful,” Diyya says. “I can go out with my friends, go on bike rides with my dad, and travel with my family. I don’t know what it would be like today without my neuro-stim.”
A high school sophomore, she plays two instruments, is active on her school’s debate team, works part-time, and is considering a potential career in medicine.
Taking an active role in her healthcare
Of her experience as a CHOC patient, Diyya adds, “It was unusual for me to have a doctor talking directly to me, and asking questions of me, and not just talking to my parents. Dr. Chogle wanted to make sure that I was comfortable with everything, not just that my parents were OK with it. He spent a lot of time with us, and never made us feel rushed.”
Through these health challenges, Diyya has learned how to take an active role in managing her overall health.
“Diyya has learned how to communicate with the school nurse and her healthcare providers effectively,” Priya says.
As a parent, Priya is grateful that her daughter has access to cutting-edge treatment. Her team also recommended acupuncture and cupping, which have served beneficial during stressful times like finals week and AP testing.
“I am so grateful that Diyya has access to a healthcare team that takes the time to research what innovative options there are for the patients. Seeing the spark in her eye come back is priceless.”
This experience has made Diyya more sympathetic of others.
“Especially since my diseases were not very visible, I learned not to judge someone based off of just their looks,” she says. “You never know what they might be going through. It’s cheesy, but it’s true.”
Get more expert health advice delivered to your inbox monthly by subscribing to the KidsHealth newsletter here.
Learn more about the gastroenterology (GI) program at CHOC
Our gastroenterology team is committed to offering patients the very latest treatments in an environment dedicated to patient- and family-centered care.





